The 2026 AHA Stroke Update: Practice-Changing Insights for Emergency Care
How the 2026 AHA Update Reshapes Emergency Stroke Management
At 2:47 AM, EMS calls in:
“72-year-old, facial droop, slurred speech, BP 210/110. Last known well 45 minutes ago.”
First: Stroke is officially a SYSTEM problem
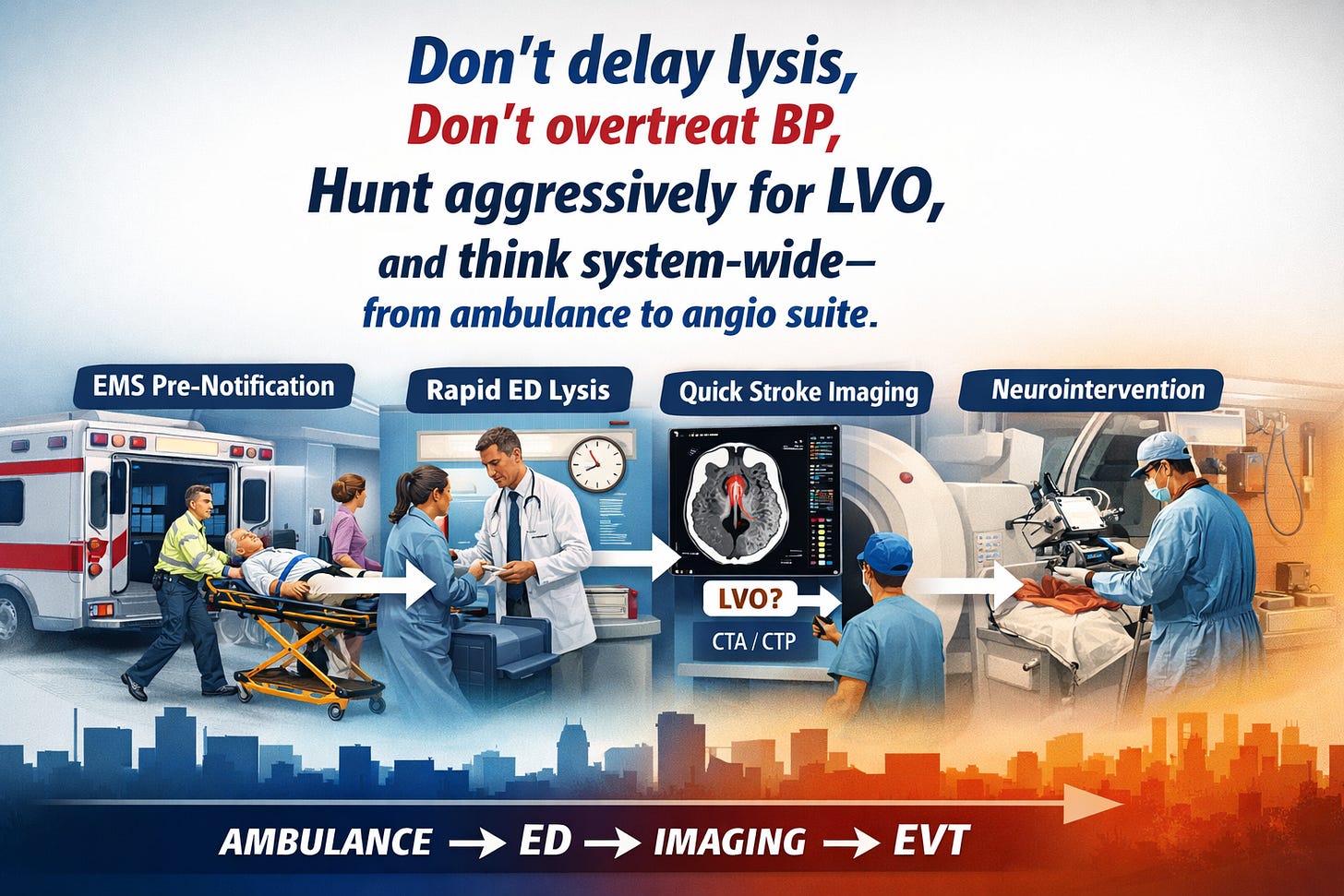
The guideline now frames care from:
🚑 Ambulance bay → 🏥 ED resus → 🧠 early ICU/ward
Emergency Medicine is named as a core driver of outcomes.
What that means practically:
• EMS pre-notification is no longer “nice to have” — it shortens door-to-CT, door-to-needle, and reduces mortality
• Prehospital stroke/LVO scales should guide smarter triage
• Patients should go directly to EVT-capable centers when systems allow
• Mobile Stroke Units are now recommended where available
👉 Faster identification beats perfect in-hospital workflows.
❌ Three things to stop doing (they don’t help)
1️⃣ Remote ischemic conditioning (BP cuff ischemia tricks) → no outcome benefit
2️⃣ Prehospital nitroglycerin patches → possible harm
3️⃣ Aggressive early BP lowering to 130–140 → doesn’t improve outcomes
💡 Hyperacute stroke patients don’t need “normal” BP — they need reperfusion.
💉 Thrombolysis just got easier (and faster)
Big wins:
✅ Tenecteplase OR alteplase are both guideline-approved
✅ Don’t delay IVT for CTA or perfusion imaging if patient is eligible
✅ Treat disabling deficits within 4.5 hours — even with low NIHSS
For mild, non-disabling strokes:
➡️ Skip thrombolysis
➡️ Start dual antiplatelets instead
Extended window up to 9 hours?
👉 Possible with advanced imaging showing salvageable brain.
Thrombectomy: many more patients now qualify
EVT isn’t just for “perfect” CT scans anymore.
The 2026 update supports EVT in selected patients with:
• Larger infarct cores
• Lower ASPECTS scores
• Some pre-existing disability
• Basilar artery occlusion up to 24 hours (strong recommendation)
👉 ED takeaway: look hard for LVO and BAO. Your CTA matters more than ever.
📉 Blood Pressure
✅ Pre- Reperfusion Target <185/110 mm Hg
✅ After IV thrombolysis (IVT)
The guideline compared:
Intensive control: SBP <140 mmHg
vsStandard control: SBP <180 mmHg
👉 No functional benefit with <140 mmHg
✔️ Recommended approach remains:
Keep SBP ≤180 mmHg and DBP ≤105 mmHg after thrombolysis
(not lower unless another indication exists)
After successful thrombectomy (EVT with reperfusion mTICI 2b–3)
Trials targeting:
👉 SBP <140 mmHg for first 72 hours
showed harm
❌ Not recommended
✔️ Use non-intensive targets (similar to post-IVT ranges)
👉 Practically: avoid pushing SBP down to 140
(maintain around ≤180 mmHg unless clinically indicated)
If not meeting Reperfusion Criteria
(Concept of Permissive Hypertension)
For acute ischemic stroke patients not receiving reperfusion therapy (IV tPA or mechanical thrombectomy), blood pressure (BP) should generally not be treated unless it is severely elevated, specifically >220/120 mmHg.
In such cases, a cautious, gradual reduction of MAP (e.g.,15% within 24 hours) is recommended to avoid hypo-perfusion.
🍬 Glucose
The guideline evaluated tight control:
❌ 80–130 mg/dL with IV insulin infusions
Result:
No improvement in 3-month functional outcome
Increased severe hypoglycemia
🚫 Not recommended
✔️ What to aim for practically in ED/early admission
The guideline doesn’t mandate a single “tight” number — just to avoid extremes.
👉 Most stroke units/ICU protocols now align with:
~140–180 mg/dL
(avoid hypoglycemia, avoid very high sugars)
🧠 Quick ED cheat summary
After IVT:
👉 BP ≤180/105 mmHg
After EVT:
👉 Don’t force SBP to 140
👉 Keep permissive (≈ ≤180/105)
Glucose:
🚫 Don’t chase 80–130
✔️ Aim moderate control (~140–180)
The 2026 AHA stroke update kills aggressive physiology control: keep BP under 180 after IVT/EVT (not 140), and avoid tight glucose targets — moderation beats micromanagement.
Pediatric stroke (👶) finally enters real-time EM practice
Key shifts:
• Adult stroke scales don’t work well in kids
• Low threshold for pediatric stroke activation
• MRI/MRA preferred (CT/CTA if MRI delayed)
• Alteplase may be considered
• EVT can help selected children — even very young ones at expert centers
👉 Stroke isn’t just an adult disease anymore.
𝗞𝗲𝘆 𝗘𝘃𝗶𝗱𝗲𝗻𝗰𝗲-𝗕𝗮𝘀𝗲𝗱 𝗖𝗵𝗮𝗻𝗴𝗲𝘀:
1️⃣ 𝗘𝗩𝗧 𝗳𝗼𝗿 𝗟𝗮𝗿𝗴𝗲 𝗜𝗻𝗳𝗮𝗿𝗰𝘁 𝗖𝗼𝗿𝗲𝘀
Meta-analysis of 6 RCTs (n=1,600+): Combined OR 1.57 (95% CI 1.40-1.76) for favorable functional outcome (mRS 0-2) with EVT vs. medical management in ASPECTS 3-5. NNT ≈7-8 for functional independence.
2️⃣ 𝗧𝗲𝗻𝗲𝗰𝘁𝗲𝗽𝗹𝗮𝘀𝗲 𝗡𝗼𝗻𝗶𝗻𝗳𝗲𝗿𝗶𝗼𝗿𝗶𝘁𝘆
Multiple trials (AcT, ATTEST, TRACE-II) demonstrated noninferiority with superior operational characteristics: 43% reduction in dosing errors, 15-minute time savings, comparable 90-day mRS outcomes.
3️⃣ 𝗕𝗹𝗼𝗼𝗱 𝗣𝗿𝗲𝘀𝘀𝘂𝗿𝗲 𝗠𝗮𝗻𝗮𝗴𝗲𝗺𝗲𝗻𝘁
ENCHANTED trial: Intensive BP lowering (SBP <140) vs. guideline-recommended (<180) showed no difference in primary outcome (death/disability) but increased renal adverse events. BLOOD-PRESSURE trial: Intensive control post-EVT associated with worse functional outcomes (adjusted OR 0.70, 95% CI 0.52-0.95).
4️⃣ 𝗚𝗹𝘆𝗰𝗲𝗺𝗶𝗰 𝗖𝗼𝗻𝘁𝗿𝗼𝗹
SHINE and TEXAIS trials: Tight glucose control (80-130 mg/dL) vs. standard (≤180 mg/dL) showed no benefit in 90-day mRS (OR 1.03, 95% CI 0.88-1.20) with 3-fold increase in severe hypoglycemia.
🧩 The new ED philosophy of stroke care
The 2026 guidelines quietly flip the mindset:
Old approach:
👉 Stabilize everything → image → think → treat
New approach:
👉 Identify fast → image fast → reperfuse fast
Avoid delays. Avoid overcorrection. Expand treatment.
References:-
Prabhakaran S, Gonzalez NR, Zachrison KS, et al. 2026 Guideline for the early management of patients with acute ischemic stroke: a guideline from the American Heart Association/American Stroke Association. Stroke. 2026;57:e00–e00. doi:10.1161/STR.0000000000000513