Etomidate in the Emergency Department
Balancing hemodynamic stability with adrenal effects
Where etomidate fits in the ED ?
Etomidate is one of the most commonly used induction agents for:
Rapid Sequence Intubation (RSI)
Short procedural sedation (e.g., cardioversion)
Its appeal lies in:
Rapid onset (10–20 sec)
Short duration (4–10 min)
Minimal cardiovascular depression
This makes it particularly valuable in critically ill or hypotensive patients, where even small drops in blood pressure can be dangerous.
Dosing essentials
RSI: 0.3 mg/kg IV (max ~40 mg)
Unstable / elderly: 0.2 mg/kg
Procedural sedation: 0.1 mg/kg
Always dose using actual body weight to avoid awareness during paralysis.
Clinical advantages
Preserves hemodynamic stability better than most induction agents
Maintains cerebral perfusion pressure → useful in head injury
Reliable intubating conditions with high first-pass success
Rapid recovery profile for short procedures
Adrenal suppression: the central controversy
Mechanism
Etomidate inhibits 11β-hydroxylase, impairing cortisol synthesis:
Leads to reduced endogenous cortisol production
Effect occurs even after a single dose
Duration:
Suppression may last 6–72 hours
Biochemical vs clinical significance
Biochemical suppression:
Almost universal → low cortisol levels after administrationClinical adrenal insufficiency:
Variable → may present as:Persistent hypotension
Increased vasopressor requirement
Key point:
Not all patients with low cortisol develop clinically significant instability.
Adrenal effects in real-world ED practice
In the emergency setting, etomidate-induced adrenal suppression is best understood as a transient physiologic trade-off rather than a definitive clinical harm.
While cortisol levels drop predictably after a single dose, most patients do not manifest overt adrenal crisis.
The effect becomes clinically relevant primarily in septic shock, where endogenous cortisol is crucial for maintaining vascular tone and catecholamine responsiveness.
In such patients, etomidate may contribute to vasopressor dependence or delayed shock reversal, even though a clear increase in mortality has not been consistently demonstrated. In contrast, in undifferentiated shock or cardiogenic instability, the immediate hemodynamic stability provided during intubation often outweighs this transient endocrine effect, making etomidate a reasonable and frequently preferred choice.
What the evidence shows
General ED population
No consistent increase in mortality after single-dose use
Benefits in maintaining hemodynamics often outweigh risks
Sepsis and septic shock
Higher rates of adrenal suppression
Increased vasopressor requirement seen in several studies
No clear mortality difference compared with alternatives
Interpretation:
The signal is physiologic (pressor need) rather than definitively outcome-driven
Other important adverse effects
Myoclonus (~30%) → limits use in procedural sedation
No analgesia → must combine with appropriate agents
Transient apnea/hypoventilation possible
Injection site pain (~20%)
Avoid repeat dosing
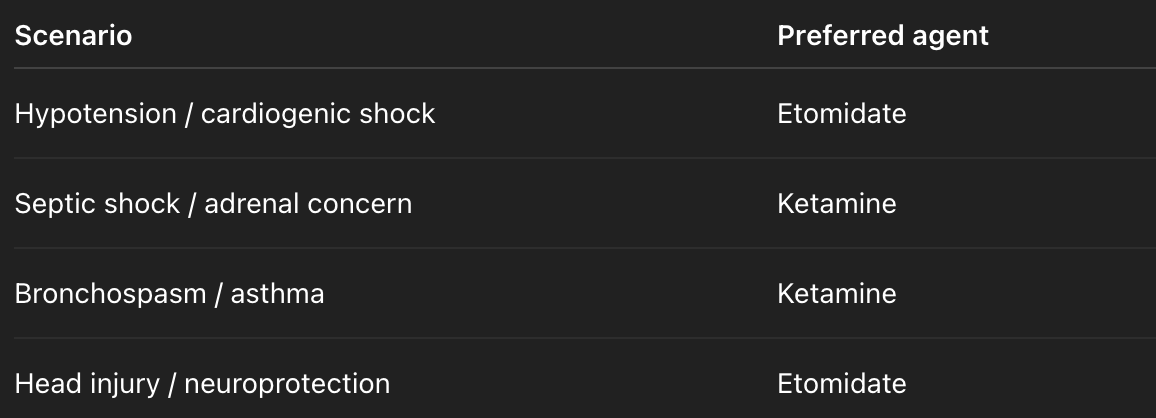
Etomidate vs Ketamine: bedside decision-making
Outcomes between agents are largely similar—choice depends on physiology and context rather than superiority
Steroids after etomidate?
Routine steroid use is not recommended
No clear improvement in outcomes
Reserve steroids for established refractory septic shock, not prophylaxis
Practical ED approach
Use etomidate when:
Patient is hemodynamically unstable
Concern for peri-intubation hypotension
Need for neuroprotection
Consider alternatives when:
Septic shock with high vasopressor requirement
Concern for adrenal insufficiency impact
Take-home message
Etomidate provides rapid, reliable, hemodynamically stable induction
It causes predictable, transient adrenal suppression
Clinical impact is usually limited, but context matters in sepsis
The decision is not about the drug alone—it’s about the patient in front of you
“Etomidate protects the pressure upfront—just be mindful of the cortisol trade-off.”